Hyperinsulinism Diagnosed
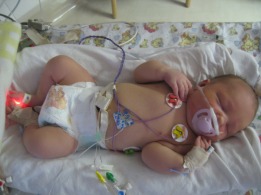
Our baby girl – Gemma Lynne Deutschmann – was born on the 8th of September 2007, and weighed a healthy 4.080kgs. The pregnancy and the birth went really well with no problems at all, so we weren’t surprised at all that she was well and healthy......... or so we thought.
Four hours after she was born, Gemma’s glucose dropped to 0, and all her body functions shut down. She stopped breathing and was immediately rushed to NICU. She was however, in God’s hands from the moment this all happened, because if the nurses noticed her just a few minutes too late, she may have suffered serious brain damage. Our pediatrician just happened to be doing his rounds in the Neonatal ICU at the time, and immediately put her on a glucose drip.
The doctor did all sorts of tests including blood tests, a lumbar puncture, etc, to rule out any other factors before she was diagnosed with Congenital Hyperinsulinism (CHI for short). It was a miracle in itself that our paediatrician had seen one other case of a boy with CHI a few months before so he was able to diagnose her within a few days.
CHI is a condition that is the exact opposite of Diabetes. Gemma’s pancreas therefore randomly secretes too much insulin and this can cause her glucose to drop to below 2.5 (a normal child’s glucose ranges between 3.5 and 8), and without the correct management could result in her going into a coma or possibly death.
The plan was for Gemma to stay in NICU for at least one month to see if there was a chance that she would grow out of this condition in a few weeks. During her first few days of her life, Gemma was fed through a glucose drip to keep her sugar stable. A few days later she was fed expressed breast milk continuously through a nose tube (Naso Gasric tube), and was on an infusion of medication called Diazoxide. After about 4 weeks she was on 3 hourly feeds and had been weaned off the medication. We were so excited, and were getting ready to take her home, as we thought she had recovered. However, her glucose dropped again, so she was put back onto the medication.
During this time, Michael had been in touch with an endocrinologist in Cape Town who was more familiar with this condition, as she specializes in the pancreas. Our doctor (who had done a fantastic job so far) told us he had done all he could for Gemma, and transferred Gemma to Cape Town after 6 weeks in Bloemfontein.
We arrived in Cape Town, and Gemma was put back on drips. We were very disheartened as we felt we were starting from scratch again. We decided to hold our heads high and put our trust in the doctors there.
With HI there are 2 major types. Type 1 is called focal HI, where just a tiny bit of the pancreas is affected, and this can be cut out, and the problem will be solved. Type 2 is called Diffuse HI, where the whole pancreas is affected, and this is usually a genetic problem. The solution for this is to either have between 95 and 98% of the pancreas removed and the baby may stand the chances of instantly becoming a diabetic, or it can be controlled by medication. In order to see which Type Gemma has we needed to do a PET-scan, but the problem was, was that this scan is only done in a few countries in the world, including Germany (Berlin). After much preparation, and with just the plane tickets to purchase, we were almost set to head to Germany to have this scan done. A day before we were going to leave, Michael phoned England to see if our DNA test results were ready (we had sent our blood samples when Gemma was a week old, and were promised to have the results back 2 weeks later). Dr Hussain (the world leader in this condition), quickly analyzed them, and told us the results showed that Gemma’s type of HI is a genetic problem, whereby the chromosome number 11 on both of our sides has a defect, and therefore she has the Diffuse type. Our trip was cancelled abruptly, and thousands of Rands were saved after that very important phonecall.
Gemma was put on a medication called Octreotide, which consists of four injections a day. It took her little body a while to adjust to this medication. Her sugar would still keep dropping and not recover after feeds, so she kept having drips put into her arms and legs. Being a big strong baby had its disadvantages, as she kept pulling them out. One of the most heartbreaking things to have seen was a drip put into the side of her shaved head. It was after she had pulled this drip out that things started getting better. Her body started responding well to the medication, and when her sugar did drop it would immediately rise after a feed.
At this stage Gemma had been in Cape Town’s NICU for about 6 weeks. She was on a constant feed during the night (through the NG tube), getting her 4 injections and being monitored every three hours. By the seventh week she had not needed a drip for two whole weeks. We were adamant that through our observations we would be able to treat her ourselves in the comfort of our own home. It didn’t take us long to learn to check her glucose and administer injections. We were even taught how to insert the Nasogastric Tube. The Cape Town doctors advised us to have a tube inserted into Gemma’s stomach as it would be much easier to handle at home, instead of the NG tube. We wanted to save Gemma having an operation, and decided to give her a chance with the NG tube, so insisted to try it that way first at home.
After three months of Gemma's hospital stay, the 6th of December 2007 was a day that our family will always remember with the greatest fondness – the day Gemma came home, 2 days before Michael’s birthday. It was a beautiful day.
Having Gemma home was a huge blessing, and we loved every minute of it – except having to insert the NG tube, as she kept pulling it out. It was very traumatic for all 3 of us as she would scream, and both Michael and myself would get very stressed out. We saw a speech therapist to get advice on why Gemma wasn’t drinking from her bottle. She told us that it could possibly be because her throat was painful, as some of the lining could have been damaged from the NG tube having to be inserted so many times. That same day we made an appointment to have a Gastric Tube inserted into her stomach, if we had of known the damage we were causing we would have done this much earlier.
She was admitted into hospital a few days later. The operation was a success and she was discharged three days later. Life with a G-tube was much easier for all of us. We could at least sleep a bit better at night knowing that she wasn't ripping her night feed out. We would still try our best to get her to drink from her bottle before giving her feeds through the tube. It would sometimes take up to 45minutes for her to drink about 10mls, of which most she spat out. During this time her blood sugars would drop even more and would get lethargic and refuse to continue. It was a no win situation.
Four hours after she was born, Gemma’s glucose dropped to 0, and all her body functions shut down. She stopped breathing and was immediately rushed to NICU. She was however, in God’s hands from the moment this all happened, because if the nurses noticed her just a few minutes too late, she may have suffered serious brain damage. Our pediatrician just happened to be doing his rounds in the Neonatal ICU at the time, and immediately put her on a glucose drip.
The doctor did all sorts of tests including blood tests, a lumbar puncture, etc, to rule out any other factors before she was diagnosed with Congenital Hyperinsulinism (CHI for short). It was a miracle in itself that our paediatrician had seen one other case of a boy with CHI a few months before so he was able to diagnose her within a few days.
CHI is a condition that is the exact opposite of Diabetes. Gemma’s pancreas therefore randomly secretes too much insulin and this can cause her glucose to drop to below 2.5 (a normal child’s glucose ranges between 3.5 and 8), and without the correct management could result in her going into a coma or possibly death.
The plan was for Gemma to stay in NICU for at least one month to see if there was a chance that she would grow out of this condition in a few weeks. During her first few days of her life, Gemma was fed through a glucose drip to keep her sugar stable. A few days later she was fed expressed breast milk continuously through a nose tube (Naso Gasric tube), and was on an infusion of medication called Diazoxide. After about 4 weeks she was on 3 hourly feeds and had been weaned off the medication. We were so excited, and were getting ready to take her home, as we thought she had recovered. However, her glucose dropped again, so she was put back onto the medication.
During this time, Michael had been in touch with an endocrinologist in Cape Town who was more familiar with this condition, as she specializes in the pancreas. Our doctor (who had done a fantastic job so far) told us he had done all he could for Gemma, and transferred Gemma to Cape Town after 6 weeks in Bloemfontein.
We arrived in Cape Town, and Gemma was put back on drips. We were very disheartened as we felt we were starting from scratch again. We decided to hold our heads high and put our trust in the doctors there.
With HI there are 2 major types. Type 1 is called focal HI, where just a tiny bit of the pancreas is affected, and this can be cut out, and the problem will be solved. Type 2 is called Diffuse HI, where the whole pancreas is affected, and this is usually a genetic problem. The solution for this is to either have between 95 and 98% of the pancreas removed and the baby may stand the chances of instantly becoming a diabetic, or it can be controlled by medication. In order to see which Type Gemma has we needed to do a PET-scan, but the problem was, was that this scan is only done in a few countries in the world, including Germany (Berlin). After much preparation, and with just the plane tickets to purchase, we were almost set to head to Germany to have this scan done. A day before we were going to leave, Michael phoned England to see if our DNA test results were ready (we had sent our blood samples when Gemma was a week old, and were promised to have the results back 2 weeks later). Dr Hussain (the world leader in this condition), quickly analyzed them, and told us the results showed that Gemma’s type of HI is a genetic problem, whereby the chromosome number 11 on both of our sides has a defect, and therefore she has the Diffuse type. Our trip was cancelled abruptly, and thousands of Rands were saved after that very important phonecall.
Gemma was put on a medication called Octreotide, which consists of four injections a day. It took her little body a while to adjust to this medication. Her sugar would still keep dropping and not recover after feeds, so she kept having drips put into her arms and legs. Being a big strong baby had its disadvantages, as she kept pulling them out. One of the most heartbreaking things to have seen was a drip put into the side of her shaved head. It was after she had pulled this drip out that things started getting better. Her body started responding well to the medication, and when her sugar did drop it would immediately rise after a feed.
At this stage Gemma had been in Cape Town’s NICU for about 6 weeks. She was on a constant feed during the night (through the NG tube), getting her 4 injections and being monitored every three hours. By the seventh week she had not needed a drip for two whole weeks. We were adamant that through our observations we would be able to treat her ourselves in the comfort of our own home. It didn’t take us long to learn to check her glucose and administer injections. We were even taught how to insert the Nasogastric Tube. The Cape Town doctors advised us to have a tube inserted into Gemma’s stomach as it would be much easier to handle at home, instead of the NG tube. We wanted to save Gemma having an operation, and decided to give her a chance with the NG tube, so insisted to try it that way first at home.
After three months of Gemma's hospital stay, the 6th of December 2007 was a day that our family will always remember with the greatest fondness – the day Gemma came home, 2 days before Michael’s birthday. It was a beautiful day.
Having Gemma home was a huge blessing, and we loved every minute of it – except having to insert the NG tube, as she kept pulling it out. It was very traumatic for all 3 of us as she would scream, and both Michael and myself would get very stressed out. We saw a speech therapist to get advice on why Gemma wasn’t drinking from her bottle. She told us that it could possibly be because her throat was painful, as some of the lining could have been damaged from the NG tube having to be inserted so many times. That same day we made an appointment to have a Gastric Tube inserted into her stomach, if we had of known the damage we were causing we would have done this much earlier.
She was admitted into hospital a few days later. The operation was a success and she was discharged three days later. Life with a G-tube was much easier for all of us. We could at least sleep a bit better at night knowing that she wasn't ripping her night feed out. We would still try our best to get her to drink from her bottle before giving her feeds through the tube. It would sometimes take up to 45minutes for her to drink about 10mls, of which most she spat out. During this time her blood sugars would drop even more and would get lethargic and refuse to continue. It was a no win situation.
